INTRODUCTION
Attempting to achieve ultimate facial and dental aesthetics can be challenging for a dentist. “Some dentists may not consider that facial aesthetics has much to do with them.”1 Nevertheless, using an interdisciplinary approach allows the practitioner to set a challenging goal to dramatically improve a patient’s facial appearance.
“Interdisciplinary treatment gives the dental team the opportunity to change, shape, or develop an individual’s appearance, character, or self-image, and at the same time provide a restoration that is functional and enduring.”2 In his article, Rodriguez Flores3 says: “Interdisciplinary treatment that combines orthodontics, implantology, and prostheses helps us to obtain good, predictable results that are stable over time, aesthetic and functional in the cases of adults with large edentulous spaces and multiple problems in dental arch.”
The goal of this article is to lay out the framework for a unique treatment philosophy. This philosophy is based on a different set of priorities in aesthetic treatment planning, which places the improvement of facial beauty and the creation of proper facial proportions and balance at the top of the list. An interdisciplinary approach, starting with dentofacial orthopedic and orthodontic treatment, allows the dentist to focus on facial appearance of the patient, instead of just treating occlusion and teeth. In his article, Jefferson4 states that: “There is a universal standard for facial beauty regardless of race, sex, and other variables and is based on divine proportion.” Thus, following this universal principle, one of the objectives of the treatment of complicated cases should be the enhancement of the patient’s external appearance.
The presence of preexisting malocclusions in adult cases requiring full-mouth rehabilitation makes the accomplishment of the above mentioned goals more challenging and difficult to implement using only one treatment modality. The cases presented in this article can be seen as an illustration of how the interdisciplinary approach can help in the planning and execution of complex treatments of patients with preexisting malocclusions. Orthodontic treatment in the beginning, with special attention to dentofacial orthopedics, will place teeth and jaws in a position that ensures the successful completion of the subsequent prosthetic phase of the patient’s full-mouth rehabilitation and greatly improve the overall aesthetic result.
CASE 1
Diagnosis and Treatment Planning
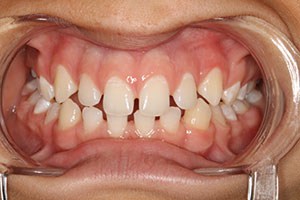
A 55-year-old female patient presented with a constricted maxilla and bilateral crossbite. Her previous request for cosmetic improvement of her smile was rejected by numerous practitioners due to very unfavorable position of her maxillary teeth (Figures 1 to 3).
Clinical analysis along with evaluation of the patient’s photographs, radiographs, and models showed that prerestorative orthodontic treatment was indicated in order to meet the patient’s expectations.
Prerestorative Orthodontic Treatment
Orthodontic treatment started with the use removable functional-orthopedic appliance (Schwarz appliance) in order to eliminate the constriction of the maxilla and bring its size into proper relation to the mandible.
Several months later, 6.0 mm expansion of the maxilla was achieved. Once the size and width of the maxilla was deemed sufficient, braces were then placed on both upper and lower arches in order to move the teeth into more favorable positions for the future restorative phase of treatment. Four months later, the objectives of this part of the treatment with braces were achieved (Figure 4) and 2 months later braces were removed (Figure 5). The new positions and relations between upper and lower teeth had become much more favorable for the planned subsequent restorative treatment. In fact, the size and shape of the maxilla changed significantly (Figures 6 and 7a and 7b). The patient’s facial appearance, occlusion, and position of her teeth had improved considerably.
 |
 |
| Figure 1. Preoperative facial view (Case 1). | Figure 2. Preoperative retracted view, in occlusion (Case 1). |
 |
 |
| Figure 3. Preoperative right lateral view, in habitual centric occlusion (Case 1). | Figure 4. Retracted view of the right side occlusion at the end of the orthodontic phase of the treatment, before removal of the brackets (Case 1). |
 |
 |
| Figure 5. Retracted view after orthodontic phase of the treatment (Case 1). | Figure 6. Preorthodontic maxillary model (Case 1). |
 |
 |
| Figure 7. (a) Postorthodontic occlusal view of the maxilla. (b) Post-ortho model of the maxillary arch (Case 1). |
Restorative Treatment
The restorative phase of treatment was initiated with the preparation of tooth No. 5 for an all-ceramic zirconia (Nobel Biocare) crown, teeth Nos. 11 to 13 (to replace existing restorations) for a 3-unit all-ceramic zirconia (Nobel Biocare) bridge, and teeth Nos. 6 to 10 for porcelain (DENTSPLY Ceramco) veneers. Then, final impressions (Flexitime [Heraeus Kulzer]) were taken and all necessary information was sent into our dental laboratory team for fabrication of the restorations.
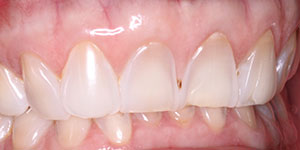
Two weeks later, the finished restorations were inserted. Zirconia crown and bridge was cemented on RelyX luting cement (3M ESPE). Porcelain veneers were cemented using 37% etch, prime and bond adhesive (DENTSPLY Caulk), and NX3 cement (Kerr). Effect of the treatment on patient’s facial appearance, occlusion, function, and aesthetics of the smile was pretty remarkable (Figures 8 and 9).
Six months after the completion of the treatment, the patient was checked and the results were found to be stable and very satisfactory to the patient (Figure 10).
CASE 2
Diagnosis and Treatment Planning
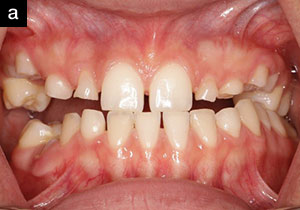
A 50-year-old male patient presented with a skeletal Class III malocclusion and anterior crossbite which adversely affected his facial appearance and ability to chew food (Figures 11 and 12). His teeth had extensive tooth structure loss due to severe grinding and erosion from pathological occlusion (Figures 13 and 14).
Clinical analysis along with evaluation of patient’s photos, radiographs, and models showed that initial orthodontic treatment was indicated in order to improve patient’s appearance, function, and smile.
To optimize the patient’s condition before restorative work was carried out, an orthodontic phase of treatment was proposed and accepted. A removable (sagittal) appliance would be used to torque his upper anterior teeth forward and also to redevelop his premaxillary area. The other goal would be to substantially open the patient’s vertical dimension in order to improve facial proportions and create necessary conditions for restorative part of full-mouth rehabilitation.
 |
 |
| Figure 8. Facial view of the patient after restorative phase of the treatment (Case 1). | Figure 9. Retracted view of the patient smile after restorative phase of the treatment (Case 1). |
 |
 |
| Figure 10. Natural smile of the patient 6 months after completion of the treatment (Case 1). | Figure 11. Preoperative facial view (Case 2). |
 |
 |
| Figure 12. Preoperative left lateral facial view (Case 2). | Figure 13. Preoperative retracted view in habitual centric occlusion (Case 2). |
 |
 |
| Figure 14. Preoperative maxillary occlusal view, showing severe wear of the teeth (Case 2). | Figure 15. Postortho facial view (Case 2). |
Prerestorative Orthodontic Treatment
Objectives of orthodontic phase of the treatment were accomplished in just 8 months. The facial appearance of the patient, his occlusion, vertical dimension, and position of his front upper teeth had changed substantially at this point of the treatment (Figure 15).
Cephalometric x-rays of the patient before and after this phase of the treatment illustrate the changes that have occurred not only in the position of the upper front teeth, but in the maxillary alveolar bone itself (Figures 16 and 17).
Restorative Treatment
The restorative phase of treatment was begun with the preparation of the patient’s maxillary and mandibular posterior teeth (teeth Nos. 4, 5, 12 to 14, 19 to 21, 28, and 29) for PFM crowns to reestablish vertical dimension of his occlusion and to restore his ability to chew. Full-mouth rehabilitation of this patient was completed by fabricating 6 zirconia all-ceramic (Nobel Biocare) crowns on teeth Nos. 6 to 11, and also in splinting the mandibular anterior teeth. Ribbond and associated with it Ribbond wetting agent and resin were used for splinting.
The effect of the treatment on the patient’s facial appearance, occlusion, function, and aesthetics of his smile was incredible and satisfying for the both patient and the doctor (Figures 18 and 19).
 |
 |
| Figure 16. Preortho cephalometric radiograph (Case 2). | Figure 17. Postortho cephalometric radiograph (Case 2). |
 |
 |
| Figure 18. Retracted view after restorative phase of the treatment was completed (Case 2). |
Figure 19. Lateral facial view after restorative phase of the treatment (Case 2). |
DISCUSSION
The prevailing treatment philosophy in general dentistry and orthodontics is based upon the assumption of immovability of the alveolar bone; after the development of the dentoalveolar complex is complete and the permanent teeth have erupted. Conventional understanding is that the labial alveolus is immovable based on research done by Engelking and Zachrisson5 and Thilander et al,6 who showed that “dehiscences or fenestrations can be produced in the buccal alveolar plate by moving teeth in a facial direction.”6 On the contrary, data from Lindskog-Stokland et al7 and Melsen,8-10 advocate that the dentoalveolar complex is much more malleable than previously believed. The interdisciplinary approach to aesthetic dentistry, as described in this article, sides firmly with the latter conception.
In their article “Beyond the Ligament: A Whole-Bone Periodontal View of Dentofacial Orthopedics and Falsification of Universal Alveolar Immutability,” Williams and Murphy11 wrote: “When a theoretical basis for manifestly successful clinical outcomes cannot be fortified by traditional orthodontic tooth movement biology (that focuses solely on the periodontal ligament as the operant organ), a new hypothesis should be built on the old. It is forces acting beyond the ligament that may be significant determinants of the alveolus and the consequent dentofacial form, which lives, thrives, and dies by the grace of dental root positions. Dentofacial orthopedic physiology of the alveolus does not deny the relevance of periodontal ligament phenomena but merely goes beyond the ligament to analyze the alveolar response to orthopedic force from a ‘whole bone’ perspective. The behavior of the bone cannot be explained totally with a periodontal pressure-tension model.”
The cases presented in this article show that the remodeling and redevelopment of the patient’s facial and dentoalveolar structures can be performed using a dentofacial orthopedics approach regardless of age. The changes undergone in patients’ faces, the size of the jaws, and the occlusion and teeth position cannot be explained by simple tooth movement but rather by response of the alveolar bone as a “whole.” A high rate of the osteoblastic/osteoclastic activity and bone turnover are contributing to the continuing adaptability of the adult dentoalveolar complex, where alveolar bone moves in conjunction with the teeth to effectively build new bone while resorbing old bone.
Orthopedic changes in patients’ jaws and their relationships are generally responsible for overall improvement in facial appearance and the creation of much better groundwork for subsequent restorative procedures.
 |
 |
| Figure 20. Computed tomography scans several months after treatment. Left image (Case 1); right image (Case 2). |
Both patients underwent computed tomography (CT) scan examinations several months after the completion of the treatment (Figure 20). The goal of this research was to evaluate the long-term effect of the completed interdisciplinary treatment on the condition and integrity of the alveolar bone and on the position and stability of the roots of the teeth within the bone.
The assessments of these images are consistent with the picture of normal alveolar bone with roots of the teeth positioned proportionally within the boundaries of the bone. There is no visible damage, dehiscences, or fenestrations in the buccal alveolar plate and no bone loss can be observed.
These CT scans illustrate the “whole bone” remodeling response to successfully performed orthodontic treatment.
CONCLUSION
An interdisciplinary approach to full-mouth rehabilitation of complex cases that may include preexisting malocclusions can result in significant enhancement of the patient’s overall facial appearance, occlusion, functional, and aesthetic aspects of the smile. This treatment philosophy gives the dentist an opportunity to assess patients in a different way, beginning with an evaluation of the patient’s overall facial beauty.
The ensuing orthodontic treatment with special attention paid to dentofacial orthopedics allows for the remodeling of a patient’s alveolar bone. The bone movement creates a proper orthopedic relationship between the jaws with stable results, regardless of the patient’s age. The addition and implementation of this phase of treatment will help to ensure that the teeth and jaws are in a more favorable position, thus dramatically improving the dentist’s chances for creating more optimal dentofacial aesthetics and better occlusal/functional results.
Acknowledgement
Author thanks Drs. Jerald Friedman and Zev Schulhof from North Jersey Oral and Maxillofacial Surgery for their help in obtaining CT Scan examinations of the patients. The author also thanks Joseph Passaro Porcelain Studio from New York, NY, for providing excellent restorations.
References
- Sarver DM. Growth maturation aging: how the dental team enhances facial and dental esthetics for a lifetime. Compend Contin Educ Dent. 2010;31:274-283.
- Winter RR. Interdisciplinary treatment planning: why is this not a standard of care? J Esthet Restor Dent. 2007;19:284-288.
- Rodriguez Flores JM. Multidisciplinary orthodontic treatment in adult patients: the future of orthodontics. Int J Orthod Milwaukee. 2010;21:11-21.
- Jefferson Y. Facial beauty—establishing a universal standard. Int J Orthod Milwaukee. 2004;15:9-22.
- Engelking G, Zachrisson BU. Effects of incisor repositioning on monkey periodontium after expansion through the cortical plate. Am J Orthod. 1982;82:23-32.
- Thilander B, Nyman S, Karring T, et al. Bone regeneration in alveolar bone dehiscences related to orthodontic tooth movements. Eur J Orthod. 1983;5:105-114.
- Lindskog-Stokland B, Wennström JL, Nyman S, et al. Orthodontic tooth movement into edentulous areas with reduced bone height. An experimental study in the dog. Eur J Orthod. 1993;15:89-96.
- Melsen B. Biological reaction of alveolar bone to orthodontic tooth movement. Angle Orthod. 1999;69:151-158.
- Melsen B. Tissue reaction to orthodontic tooth movement—a new paradigm. Eur J Orthod. 2001;23:671-681.
- Melsen B. Dr. Birte Melsen on adult orthodontic treatment. Interview by Vittorio Cacciafesta. J Clin Orthod. 2006;40:703-716.
- Williams MO, Murphy NC. Beyond the ligament: a whole-bone periodontal view of dentofacial orthopedics and falsification of universal alveolar immutability. Seminars in Orthodontics. 2008;14:246-259.
Dr. Rubinov graduated from New York University (NYU) College of Dentistry in 1992. He is also a foreign trained dentist who received his dental degree in Leningrad, Russia in 1974. In 1984 Dr. Rubinov obtained a PhD degree in dentistry in Leningrad. Dr. Rubinov is an active member and instructor of International Association for Orthodontics, Member and Fellow of the American Association for Functional Orthodontics, and is clinical assistant professor of NYU College of Dentistry. Dr. Rubinov maintains a full-time private practice in Cliffside Park, NJ, providing cosmetic dentistry along with orthodontics for children and adults and TMJ treatment. He can be reached at (201) 941-8877, at drrubinov@yahoo.com, or at realsmile.com.
Disclosure: Dr. Rubinov reports no disclosures.